Remember the cheesy John Travolta-Nicolas Cage action flick Face Off? Well, it seems as if the face transplant technology featured in the film could soon be a reality.
The results of a new study on human face transplantation were recently presented at the yearly meeting of the Radiological Society of North America (RSNA). The study was led by Darren M. Smith, M.D., plastic surgery resident at the University of Pittsburgh Medical Center (UPMC), and it offers hope to victims of serious facial injuries.
The traditional problem with face transplants is that serious injuries or defects are nearly impossible to correct using traditional surgery.
In a face transplant, tissue from a donor is used to rebuild glaring flaws and restore important physical functions like breathing, chewing and speaking. Of course, surgeons also attempt to restore a normal appearance.
“This surgery is for patients with devastating injuries to the face, who have lost their ability to smell, eat and engage socially and have no other conventional treatment options,” said Vijay S. Gorantla, M.D., Ph.D., administrative medical director of the Reconstructive Transplantation Program at UPMC.
As such, understanding the multifaceted tissue defects caused by life threatening facial damage like electric burns, blast wounds and other trauma is important for both technical success and analysis of the return of function after the transplant.
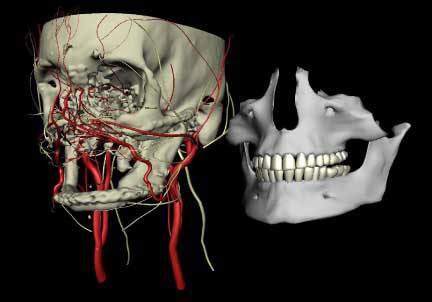
According to Gorantla, gathering information from multiple 3D imaging exams allowed researchers to better evaluate the facial structure and contours, the underlying bone, muscles, nerves and vessels, as well as the extent of damage.
Sophisticated computer modeling software came into play and was used to help Drs. Smith and Gorantla, along with Joseph Losee, M.D. to create a 3D model of the patient’s head and neck anatomy. Similar modeling technology is frequently used in Hollywood to generate computer-generated characters with detailed three-dimensional human features and realistic expressions.

“We have integrated data from multiple imaging sources into a single 3D representation that allows for real-time user interaction and modification,” explained Smith.
“In assessing eligibility for this procedure, it is critical to understand whether the patient has enough blood vessels and bone structure to support new facial tissue. This 3D modeling helps us customize the procedure to the patient’s individual anatomy so that the donor tissue will fit like a puzzle piece onto the patient’s face.”
The team also used computer modeling to overlay the patient model with a polygon mesh of a generic human face and tweaked it to fit the recipient. Dr. Smith said the ability to control this 3D facial envelope over the face model allows the surgical team to be a part of planning exactly where bone, blood vessel and nerves will be cut and connected.
It also provide them with the useful ability to evaluate the possible outcomes of reconstructive transplantation, including nerve regeneration inside the transplanted facial tissue.
“The goal of face transplantation is not just structural,” Dr. Gorantla said. “It is about restoring function, so that patients are once again able to chew their food, smile and regain the most important aspect of a normal face – [in essence], to [once again] look human.”






